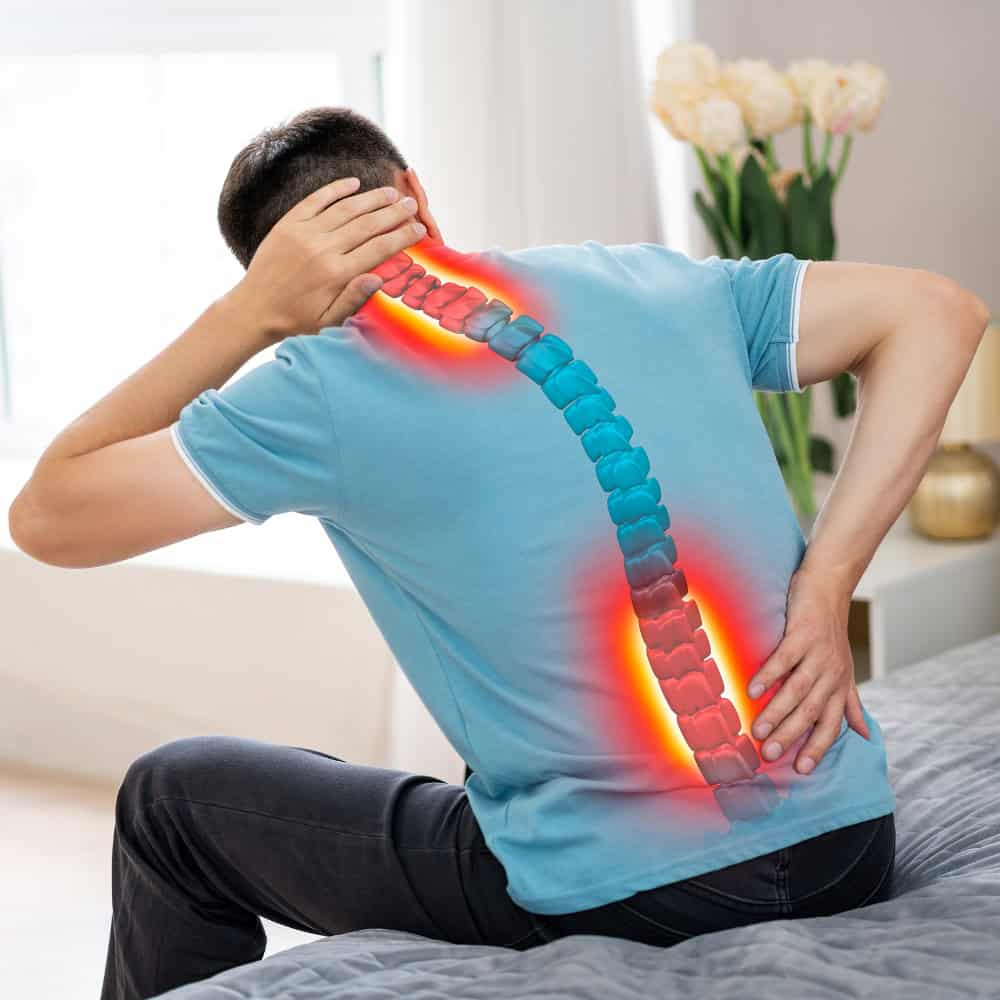
Repetitive Strain Injury (RSI): Causes, Symptoms, and Evidence-Based Recovery
Repetitive strain injury (RSI) is a broad term for musculoskeletal disorders caused by repeated movements, sustained postures, or prolonged physical stress. Whether you’re typing at a desk, operating machinery, or practicing an instrument, microtrauma to muscles, tendons, and nerves can accumulate over time.
Left unaddressed, RSI can progress from mild discomfort to chronic pain that disrupts work, sleep, and daily function. The good news? With early recognition, targeted treatment, and ergonomic adjustments, most people recover fully and prevent recurrence.
What Is Repetitive Strain Injury (RSI)?
Repetitive strain injury, also known as repetitive stress injury or work-related upper limb disorder, isn’t a single diagnosis. It’s an umbrella classification for overuse conditions affecting soft tissues—primarily tendons, muscles, and nerves. Common clinical labels under the RSI spectrum include tendonitis, tenosynovitis, bursitis, and nerve compression syndromes like carpal tunnel syndrome.
At the cellular level, RSI develops when repetitive microtrauma outpaces the body’s natural repair cycle. Inflammation builds, connective tissue stiffens, and nerve pathways become sensitized. Without intervention, this inflammation cycle can lead to chronic pain, reduced range of motion, and long-term functional limitations.
Common Causes & Risk Factors
RSI rarely stems from a single incident. It’s typically the result of cumulative exposure to biomechanical stressors. Key contributors include:
- Repetitive Motions: Typing, clicking, scanning, assembly line work, or musical instrument practice
- Poor Posture & Ergonomics: Slouched seating, unsupported wrists, screens positioned too high or low
- Forceful Exertions: Heavy lifting, gripping tools tightly, or applying constant pressure
- Static Loading: Holding the same position for extended periods without micro-breaks
- Environmental Factors: Cold temperatures, vibration exposure, or inadequate workstation lighting
Certain populations face higher susceptibility. Office workers, gamers, musicians, healthcare professionals, and manufacturing employees report the highest incidence rates. Age, pre-existing joint conditions, pregnancy, and metabolic factors like diabetes can also lower tissue resilience and accelerate symptom onset.
Key Symptoms to Watch For
Early RSI symptoms are often subtle, making them easy to dismiss as normal fatigue. Recognizing warning signs early dramatically improves recovery outcomes. Common indicators include:
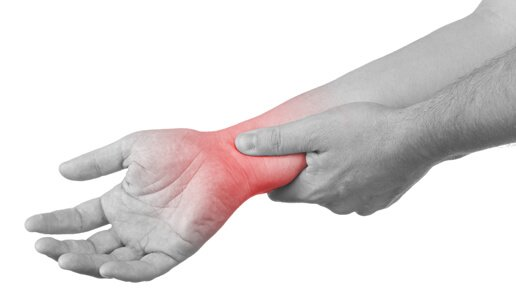
- Aching or Throbbing Pain: Localized to wrists, forearms, elbows, shoulders, or neck
- Stiffness & Reduced Mobility: Difficulty gripping, typing, or rotating joints
- Tingling or Numbness: Often signals nerve involvement, particularly in the hands and fingers
- Weakness: Dropping objects, decreased grip strength, or fatigue during routine tasks
- Sensitivity to Touch or Temperature: Inflamed tissues often react sharply to cold or pressure
- Nighttime Disruption: Pain or tingling that wakes you up is a strong indicator of progressive nerve or tendon irritation
Symptoms typically worsen with continued activity and improve with rest. If discomfort persists beyond a few days or begins interfering with daily tasks, it’s time to intervene.
How RSI Is Diagnosed
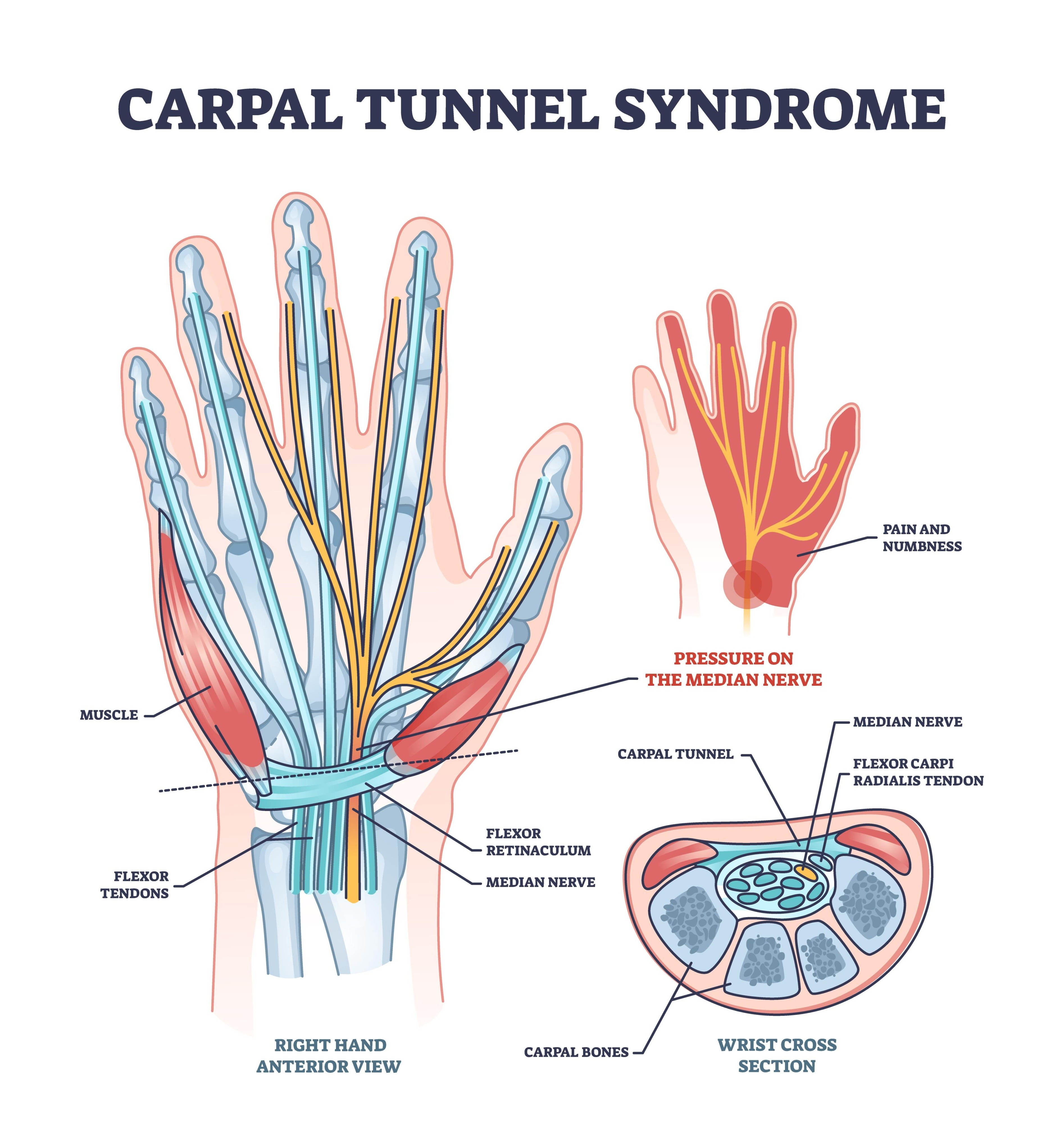
Accurate diagnosis is critical because treatment pathways vary based on whether tendons, muscles, or nerves are primarily affected. A qualified healthcare provider will typically conduct:
- Clinical History & Movement Assessment: Tracking symptom patterns, work habits, and aggravating/relieving factors
- Physical Examination: Palpation, range-of-motion tests, grip strength measurement, and nerve tension screens
- Provocative Tests: Phalen’s or Tinel’s tests for carpal tunnel, resisted movement tests for tendonitis
- Imaging & Diagnostics: Ultrasound for soft tissue inflammation, X-rays to rule out arthritis or fractures, nerve conduction studies (EMG/NCS) if neuropathy is suspected
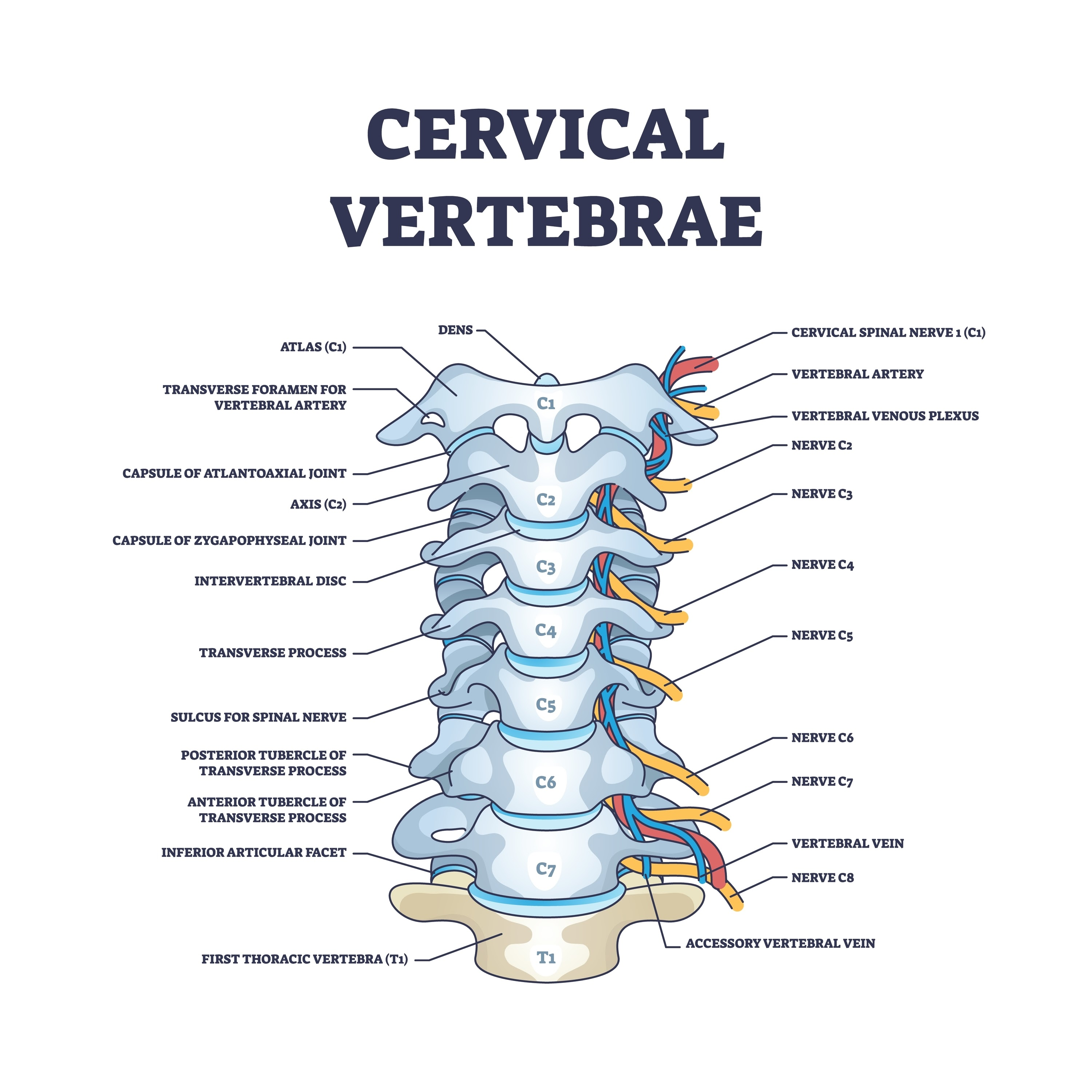
Differential diagnosis is essential. Conditions like cervical radiculopathy, thoracic outlet syndrome, or autoimmune arthritis can mimic RSI but require distinct treatment protocols.
Proven Treatment & Recovery Strategies
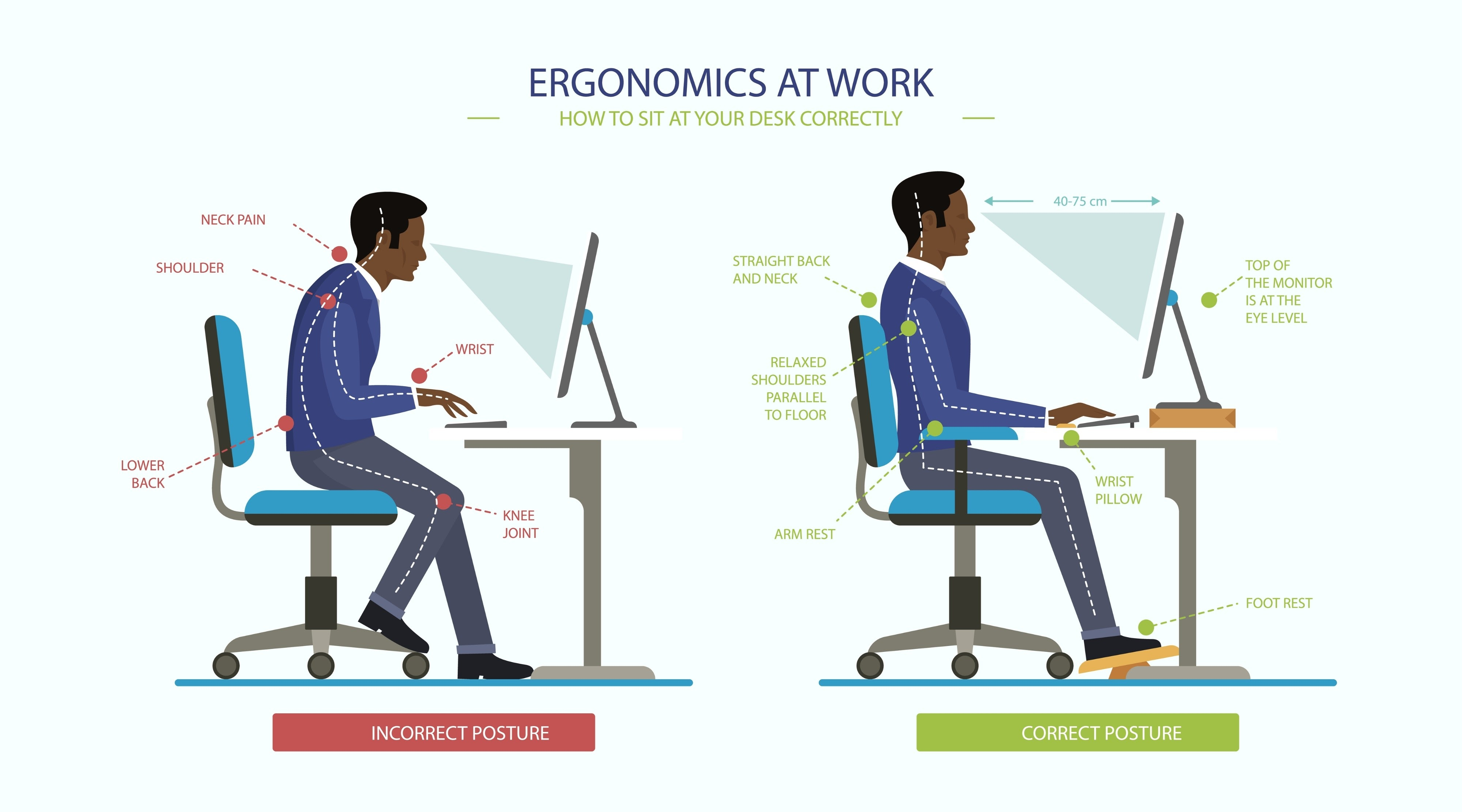
RSI recovery follows a phased approach: reduce inflammation, restore mobility, rebuild strength, and modify movement patterns. Evidence-based interventions include:
Phase 1: Acute Symptom Management
- Relative Rest: Modify, don’t eliminate, aggravating activities. Complete immobilization often delays healing.
- Ice & Heat Therapy: Ice for acute flare-ups (10–15 mins), heat for chronic stiffness and muscle relaxation.
- NSAIDs & Topical Analgesics: Short-term use to break the inflammation cycle under medical guidance.
- Bracing or Splinting: Wrist or forearm supports can reduce tendon load during recovery.
Phase 2: Mobility & Tissue Remodeling
- Physical Therapy for RSI: Targeted stretching, myofascial release, and joint mobilization restore tissue elasticity.
- Eccentric Exercises: Slow, controlled lengthening movements rebuild tendon resilience and stimulate collagen realignment.
- Nerve Gliding Techniques: Gentle flossing exercises improve nerve mobility and reduce compression-related tingling.
Phase 3: Strength & Functional Reintegration
- Progressive Loading: Gradual resistance training rebuilds grip, forearm, and shoulder stability.
- Movement Retraining: Coaching on posture, keystroke mechanics, and tool handling prevents compensation patterns.
- Workplace Modifications: Adjustable desks, ergonomic keyboards, mouse alternatives, and scheduled micro-breaks sustain recovery.
Most mild-to-moderate cases improve within 4–12 weeks with consistent intervention. Chronic or severe RSI may require 3–6 months of guided rehabilitation.
Prevention Tips for Long-Term Joint & Muscle Health
RSI is highly preventable when proactive habits replace reactive treatment. Integrate these strategies into your daily routine:
- Follow the 20-8-2 Rule: Every 30 minutes, spend 20 minutes seated, 8 minutes standing, and 2 minutes moving/stretching.
- Optimize Ergonomics: Keep wrists neutral, elbows at 90–110°, screens at eye level, and feet flat on the floor.
- Use Ergonomic Tools: Split keyboards, vertical mice, pen grips, and anti-fatigue mats reduce cumulative strain.
- Strengthen Supporting Muscles: Scapular stabilizers, rotator cuff, and forearm extensors absorb repetitive load.
- Prioritize Recovery: Hydration, sleep, and anti-inflammatory nutrition (omega-3s, magnesium, turmeric) support tissue repair.
Prevention isn’t about working less—it’s about working smarter. Small, consistent adjustments yield exponential long-term benefits.
When to See a Specialist
Not all RSI responds to self-care. Seek professional evaluation if you experience:
- Symptoms lasting longer than 2–3 weeks despite rest and modification
- Progressive weakness, muscle atrophy, or frequent object dropping
- Constant numbness, burning pain, or nighttime awakening
- Pain radiating from the neck or shoulder down the arm
- Inability to perform work or daily tasks without significant discomfort
A physiotherapist, occupational therapist, or sports medicine physician can design a personalized rehabilitation plan. Early intervention prevents chronicity and reduces the likelihood of surgical consultation.
Frequently Asked Questions About RSI
What’s the difference between repetitive strain injury and carpal tunnel syndrome?
Carpal tunnel syndrome is a specific nerve compression condition affecting the median nerve. RSI is an umbrella term that includes carpal tunnel, tendonitis, bursitis, and other overuse disorders.
How long does it take for RSI to heal?
Mild cases typically improve in 4–8 weeks with proper rest and therapy. Moderate to chronic RSI may require 3–6 months of structured rehabilitation. Consistency and ergonomic adjustments are critical.
Can repetitive strain injury be cured permanently?
Yes, most people achieve full recovery when they address underlying biomechanical stressors, complete physical therapy, and maintain preventive habits. Without lifestyle changes, recurrence is common.
Is heat or ice better for RSI pain?
Use ice for acute flare-ups (first 48–72 hours) to reduce inflammation. Use heat for chronic stiffness or muscle tension to improve blood flow and tissue elasticity.
Does typing cause repetitive strain injury?
Prolonged typing without ergonomic support, breaks, or proper technique can contribute to RSI. The risk increases with poor posture, high keystroke volume, and inadequate wrist support.
Take the Next Step Toward Pain-Free Movement
Living with repetitive strain injury doesn’t have to be your new normal. With the right assessment, targeted therapy, and ergonomic strategy, you can restore function, eliminate pain, and return to the activities you love—without fear of flare-ups.
🔹 Ready to break the cycle of repetitive stress?
📅 Book a Free 15-Minute RSI Screening Call with our certified musculoskeletal specialists. We’ll analyze your workstation habits, identify your primary stressors, and map out a personalized recovery roadmap. No guesswork. No generic advice. Just science-backed strategies tailored to your body and your routine.
👉 Schedule Your Free RSI Assessment Now
Limited spots available weekly. First consultation includes a custom ergonomic checklist + 3 targeted recovery exercises you can start today.